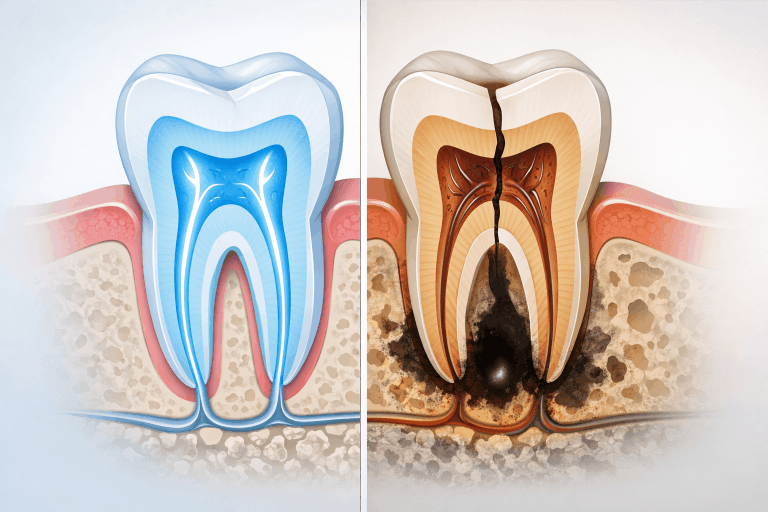
Root Canal Is Not Recommended
Root canals have been on my mind a great deal lately — and apparently on the minds of many of my patients as well, since we have seen a notable number this month.
Last post, I discussed how I determine whether a tooth can be successfully treated with root canal therapy. The short version: most of the time, saving a tooth is absolutely possible.
There’s also some exciting new science worth mentioning. A recent clinical study from King’s College London found that successful root canal treatment may offer health benefits that go well beyond saving a tooth. Patients who underwent successful therapy showed reduced glucose levels, reduced inflammation, and improved lipid profiles — markers associated with heart disease and diabetes. The purpose of root canal therapy is to correct infection or inflammation at the root of a tooth, but those are welcome side benefits.
Now, with all of that good news on the table, let’s talk about the other side of the equation. There are situations where root canal therapy is simply not the right call — and in today’s column, I want to be straightforward with you about what those situations are.
The Primary Goal of Root Canal Therapy
Before we discuss when a root canal is not recommended, it helps to understand the goal. Root canal therapy removes infected or inflamed tissue from inside the tooth, eliminates the source of pain, and allows the tooth to remain functional in your mouth.
According to the American Association of Endodontists, more than 15 million root canals are performed each year — and the vast majority are successful. My first instinct is always to keep your natural tooth. But sometimes, that simply isn’t the best path forward for your long-term dental health.
Four Reasons I May Advise a Root Canal Is Not Recommended
1. The Tooth Cannot Be Rebuilt Afterward
One of the most common questions I hear from patients is: “Is there enough tooth left to fix?” Most of the time, the answer is yes. Modern dental techniques allow us to rebuild a functional tooth with surprisingly minimal remaining structure. But there are real limits to what’s possible.
When a tooth is so severely broken or decayed that there is insufficient structure left to reconstruct it, performing root canal therapy doesn’t make sense — even if I could technically complete the procedure successfully. Treating the canal but being unable to restore the tooth afterward isn’t a solution; it’s an incomplete one. In those cases, we need to talk about extraction and replacement options, which we cover in detail on our dental services page.
2. The Infection Is Too Large to Drain Through the Tooth
When a patient comes in with significant facial swelling, that’s a serious situation that demands a different approach. One of the goals of root canal therapy is to eliminate the infection, and that happens through a small access point inside the tooth. With a moderate infection, that works well. But with a massive infection, the drainage simply cannot occur adequately through that channel.
In these cases, extracting the tooth creates a much more effective pathway for the large volume of fluid to drain. It’s not the outcome any of us wants, but it’s the right one. The Cleveland Clinic notes that untreated dental infections can spread beyond the tooth — another reason why acting quickly and choosing the right treatment matters.
3. There Is a Fracture Within the Root
A fracture inside the root of a tooth creates a fundamental problem: it prevents us from achieving the sealed, sterile environment that root canal therapy requires to be successful. Without that isolation, the tooth cannot heal properly, and the procedure will not produce the intended outcome.
When the fracture is deep and runs vertically along the root, the situation is even more clear-cut — that tooth cannot be adequately maintained in the mouth. Attempting to treat it would only delay an inevitable extraction while adding unnecessary cost and discomfort for you. As I discussed in my article on root canal longevity, fractures are one of the leading reasons treated teeth ultimately fail over time.
4. Severe Periodontal Disease Has Compromised the Tooth’s Foundation
We often think about tooth decay as the primary enemy of our teeth, but periodontal disease — disease affecting the gums and supporting bone — is equally destructive. The entire purpose of root canal therapy is to save a tooth. But if severe periodontal disease has already significantly undermined the gum and bone support around that tooth, saving it may not be realistic regardless of how well the root canal itself goes.
In the presence of advanced periodontal disease, a tooth may be headed toward loss no matter what we do to the canal. In those situations, it’s more prudent to discuss tooth replacement options like implants than to invest in a procedure that cannot address the underlying problem. The American Academy of Periodontology offers a good overview of how periodontal disease progresses and why bone support is so critical to long-term tooth retention.
What Happens After a Tooth Cannot Be Saved?
Extraction is never my first recommendation — but when it is necessary, it’s the beginning of a conversation, not the end of one. Missing teeth create their own set of problems: shifting of neighboring teeth, bone loss, changes in your bite, and long-term impact on your oral health. That’s why we discuss replacement options at the same time we discuss extraction. Dental implants, in particular, are among the most effective long-term solutions, and I’ve been placing and restoring them since the early 1990s.
Key Takeaways
- Root canal therapy is the right choice in most cases — but not all
- An unrestorable tooth, a massive infection, a root fracture, or advanced gum disease may each make root canal treatment inadvisable
- Extraction isn’t failure — it’s sometimes the most responsible clinical decision
- The conversation doesn’t end at extraction; replacing the tooth matters for your long-term health
Frequently Asked Questions
Can a dentist refuse to do a root canal?
Yes — a dentist may recommend against root canal therapy when it is not in the patient’s best clinical interest. The four most common reasons include an unrestorable tooth, an infection too large to drain through the tooth, a root fracture, or advanced periodontal disease.
Is tooth extraction always the alternative to a root canal?
In many cases, yes. When a root canal is not appropriate, extraction is often the most effective way to eliminate infection and protect surrounding teeth. Following extraction, we typically discuss replacement options such as dental implants or bridges.
Does periodontal disease prevent root canal treatment?
Severe periodontal disease can make root canal therapy inadvisable. Even if the canal itself can be successfully treated, the tooth may eventually be lost due to inadequate bone and gum support — making the procedure a poor investment.
What should I do if I’m unsure about a root canal recommendation?
Call our office. I’m always happy to review your specific situation and help you understand your options. You can reach us at 440-951-7856.
My first choice — always — is to keep your natural tooth. But sometimes the most caring thing I can do is help you see clearly when that option isn’t available, and to make sure you understand what comes next. If a tooth is bothering you or you’ve been told you may need a root canal, give us a call at 440-951-7856. Let’s sit down together and figure out the best path forward.
Jeffrey Gross, DDS, FAGD, is an Ohio-licensed general dentist and is on the staff of Case Western Reserve School of Dental Medicine.